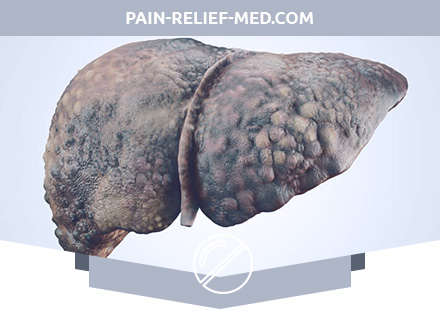
What is Alcoholic Liver Cirrhosis?
Alcoholic cirrhosis is a direct result of ethanol-induced necrosis of the parenchyma, fibrosis and nodular rearrangement of the liver.
Cirrhosis develops in approximately 10% of patients who abuse alcohol. The process usually develops slowly, and the prognosis with it is much better than with other forms of cirrhosis. M. Baillie in 1793 for the first time pointed out the connection between alcohol use and the development of cirrhosis of the liver.
Pathogenesis during Alcoholic Cirrhosis
Inflammatory reaction in connective tissue septa is negligible. Necrosis, leading to cirrhosis, may begin centrallobular or be bridge-like, extending from the center of the lobule to its periphery. In the initial stage, cirrhosis is usually micro-nodular. The formation of nodes occurs relatively slowly due to the inhibitory effect of ethanol on the regeneration of the liver. The possibility of the formation of alcoholic cirrhosis without morphological signs of inflammation through the stage of perivenular fibrosis is not excluded. In the later stages, cirrhosis often acquires the features of a macronodular one.
Symptoms of Alcoholic Cirrhosis
Features of clinical manifestations
Clinic of alcoholic cirrhosis is very diverse. Often compensated cirrhosis can remain asymptomatic and manifest slightly pronounced nausea, fatigue, and general weakness. With decompensation observed jaundice, edema, ascites, increased bleeding, disorder of consciousness. Hepatomegaly is determined in all patients, in 25% – splenomegaly. Characteristic hepatic signs are noted with varying frequency, among which Dupuytren’s contracture, gynecomastia, and “alcoholic stigmas” – dilatation of the nasal vessels and sclerae, parotid gland enlargement deserve attention. There are multiorgan lesions characteristic of chronic alcohol intoxication, manifested by peripheral polyneuropathy, encephalopathy, myocardiodystrophy, chronic pancreatitis, nephropathy, and other nosological forms.
Diagnosis of Alcoholic Cirrhosis
Diagnostic features
Diagnosis of alcoholic cirrhosis is largely based on history data. In some cases it is advisable, if possible, to apply for anamnestic data to other persons (family members of the patient). In addition, a number of questionnaires have been proposed for this diagnosis, of which CAGE deserves attention:
- Have you ever felt the need to reduce alcohol consumption?
- Are you annoyed when others criticize your drinking?
- Do you feel guilty after taking alcohol?
- Is it difficult for you to wake up the next day after taking alcohol?
A positive answer to each question is assigned 1 point. A total of 2 or more points indicates a hidden addiction to alcohol.
Laboratory indicators in patients with alcoholic cirrhosis are no different from those in patients with alcoholic hepatitis. At the same time, with latent cirrhosis, an increased level of bilirubin or changes in the activity of amino transferase may be absent. There is hypoalbuminemia, hypergammaglobulinemia, increased IgA. Confirmation of the diagnosis is possible using histological examination of liver biopsy specimens. There are signs of small-node cirrhosis with the deposition of fat of varying severity, the phenomenon of alcoholic hepatitis in patients who abuse alcohol.
Treatment of Alcoholic Cirrhosis
Treatment of alcoholic liver damage
The most important event in the treatment of any type of chronic alcoholic liver damage is the complete cessation of alcohol intake, and the compensation of protein, vitamin deficiencies, and minerals. A diet with an increase in protein content is recommended (1-1.5 g per 1 kg of the patient’s body weight). In the presence of narcological indications, social rehabilitation of alcoholics is necessary.
Treatment with coenzyme, metabolic and multivitamin preparations is indicated.
Recommended treatment is Forsliv. The composition of the drug and the form of release: 1 capsule:
- 150 mg ademetionine;
- 90 mg arginine;
- 70 mg thioctic acid.
Method of application Forsliv: 2 capsules per day. Special instructions: given the tonic effect, it is recommended to take in the morning.
Heptral (adenosyl-alfamethionine) is widely used, which reduces the degree of mitochondrial damage and helps to restore glutathione.
The absence of a cholestatic component is an indication for a course of intravenous injections of Essentiale by 5-10 ml in 3% glucose solution, 10-30 injections. At the same time, Essentiale is ingested by 2 drops. 3 times a day for 1-2 months and then 3-4 cape. per day up to 3-6 months
Showing membrane stabilizing drugs; legalon and boats for 1-2 months under the control of the functional state of the liver.
The exacerbation of alcoholic hepatitis is an indication for the treatment of detoxification therapy (intravenous drip effects of a 5% glucose solution, hemodesis, Ringer’s solution).
Glucocorticoids should be considered as an important part of the treatment of patients with severe autoimmune disorders, manifestations of encephalopathy in the absence of signs of gastrointestinal bleeding. A 4-week course of methylprednisolone at a dose of 32 mg per day, which reduces the mortality of patients during the first month, is almost complete for patients with severe hepatitis. when the value of the coefficient Maddrey> 32.
The use of UDCA in combination with antioxidants (vitamin C, B, E, polyene) is considered promising, which helps to reduce the level of aminotransferases – to reduce collagen formation. The effectiveness of UDCA preparations is probably related to their ability to inhibit the activity of proinflammatory cytokines and to have an antishostatic effect due to the stimulation of exocytosis by activating Ca-dependent α-protein kinase and a decrease in the concentration of bile acids that are toxic to the hepatic cell (cholic, lithocholic, deoxycholic) For treatment in patients with alcoholic damage to the liver, such effects of this group of drugs as immunomodulatory, hepato-protective, reducing in Aries Gender and enhancing antioxidant protection.
There is evidence of the effectiveness of anabolic steroids: colchicine, silymarin, D-penicillamine, propylthiouracil, naltrexone.
In the treatment of alcoholic liver damage using the drug metadoxil (metadoxine) in a dose of 500 mg 3 times a day for at least 3 months. Its intake normalizes the balance of free saturated and unsaturated fatty acids in plasma, which prevents the occurrence of primary structural degeneration of hepatocytes. Metadoxyl inhibits collagen synthesis, activates the processes of oxidation and elimination of ethanol and acetaldehyde.
In fatty hepatosis, duphalac administration is beneficial.
The use of anti-lipidemic drugs in patients with alcoholic liver damage is ineffective.
In the terminal stages of the disease, the only effective treatment is liver transplantation. A necessary condition for transplantation is a 6-month withdrawal period before it is performed. According to the literature, from 10 to 80% of patients after liver transplantation return to alcohol.
Forecast
Favorable subject to the refusal of alcohol intake. The worst prognosis in patients with acute alcoholic hepatitis, developed on the background of cirrhosis. Adverse histological features include intrahepatic cholestasis and perivenular fibrosis.